In September, Craig and I were married at our friends' lakeside home in Idaho! It was a magical few days on Coeur d'Alene with our families (and our Charlie girl). I did my very best to push my pain aside and soak up every moment that we'd been waiting so long to experience and share. It was truly everything we had hoped for and then some.
Photos by Don and Julia Photography
Our wedding week was followed by the most amazing road trip through Idaho, Montana, and Wyoming. We made stops through Whitefish, Glacier National Park, Bozeman, Yellowstone, Jackson Hole, and the Grand Tetons. Photos simply cannot capture how stunningly beautiful that slice of America is (though it didn't stop me from trying). And for as adventure-packed as our entire trip was, it was also entirely low-key and relaxing. No set itinerary and plenty of time for R&R, which was perfect.
And now for the head stuff.
I had to revisit that post just now to remind myself how I was even feeling then. I'd almost forgotten that although my regular frontal/temporal pain was still quite high, I was feeling complete relief in my occipital/upper cervical area. These latter spots are what I've always referred to as the "focal points" and "drivers" of my headache, so I was feeling quite optimistic. I'd also talked about the sensations I was having throughout my scalp, which consisted of the (expected) numbness (especially on the right side) and a less familiar soreness over the top that I had described as the feeling of a hammer bruising my head. Lastly, I mentioned some classic symptoms of nerve regeneration, like "pulsing," itchiness, and overall tenderness.
SO, here's the fast-forward four month update on all of that:
I'm still experiencing my frontal/temporal pain. I've spent some days on the lower end of what I call my "normal pain range," some days on the extraordinarily high end, and most days somewhere in the middle. So I can't really say that I've trended better or worse with this pain.
At around the two month mark or so, my occipital/upper cervical hot spot returned on the left side, right about where my LON is. The right side still feels good.
My scalp numbness has subsided, though I still have a weird sensation on the right side. The best way I can describe it, which may only resonate with the ponytail wearers among us, is a more amplified version of that feeling you get when you have your hair pulled up too long and then you take it down and your scalp just feels very tender. This honestly doesn't bother me though (in no way classified as "pain" in comparison to my actual head pain) and I assume it'll probably continue improving as the months go on.
So what does this status report mean?
I know, both from talking to Dr. Peled as well as other patients who've been down this path, that four months post-op is not necessarily indicative of my "final result." Nerves can take a long time to heal, which I was and still am prepared for. That being said, we would have hoped to see more progress at this point.
In the meantime, I haven't really had much luck in managing the pain. Given my track record of failing to respond to pretty much any pain medication, that's not entirely surprising. I was taking this Charlotte's Web CBD oil and had started a course of Celebrex, which wasn't touching my pain and was upsetting my stomach too much to continue. After surgery, I had also gone back on the Low-Dose Naltrexone that I talked about back in June because I wanted to make sure I had given it at least a few months. But since I didn't notice any benefit, I've since come off of that too. Craig had periodically been giving me Toradol injections to help take the edge off during extreme flare ups, but those seem to upset my stomach more too more than they help my pain (and it's really not good to take on a regular basis anyway).
Here's the arsenal of meds that came with us on our wedding road trip. Nothing says love like a shot in the ass on your honeymoon, am I right?
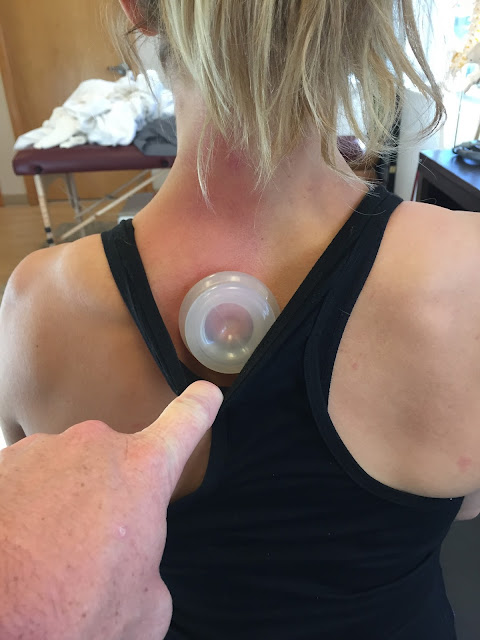
So my pain management, or "sanity maintenance," as I think more aptly describes it, has consisted of just taking care of my body and mind the best way I know how: eating a whole-foods/anti-inflammatory diet, getting daily exercise, fresh air, having a constant supply of ice packs at my disposal, and adequate sleep (including the essential afternoon nap). I've had some soft tissue work here and there, but quite honestly, don't feel any relief from it so it hasn't been a regular part of the routine lately.
I've also been dealing with even more than usual pain and tightness alongside my thoracic spine. My PT thinks this is actually my long thoracic nerve that's flared up, which makes sense given how much pain and tightness is going on above it. I know this is reactionary to that tension in my left occipital/upper cervical.
I'm also scheduled for my third course of Botox injections with my neurologist next week. I was tempted to cancel it because it obviously hasn't done anything for me over the nine month period, but I want to make sure I give it a fair chance and the data says it can take up to three rounds.
Patience aside, I had been concerned about the return of this one focal point of pain on the left side, and after talking with Dr. Peled about the nature and location of that pain, we decided there was a good chance that my left LON was still an issue, which is entirely possible given that it was just decompressed and not fully excised. So last month, Craig and I flew back to San Francisco so he could give me a nerve block to see if we could identify it as a remaining pain source.
After taking an initial look under ultrasound, he blocked that nerve with a local anesthetic just like he had done as the diagnostic procedure a few days before my surgery in July. The first injection brought my pain down a little, which gave him some guidance to tweak the location of the next one just slightly, and that time, I knew we had hit "the spot." Although very much temporary (about a half hour this time), I felt elimination of the pain at that nerve and a significant enough reduction in the frontal pain to warrant a conversation about the next step: did I want to wait things out for another few months or did I want to just move forward with an excision of this LON?
Craig and I spent the next few days talking about it before deciding that another surgery sooner rather than later made the most sense. I can understand how this might not be the right choice for everyone in my position, but the only thing I can do is listen to my body and do what feels right. And this is what feels right. So in a few weeks, I'm scheduled for surgery.
My recovery timeline will be similar to my last in that I'll have to really take it easy for about six weeks before easing my way back into light activity. Although, I'll only have one incision this time compared to the five I had before and surgery will obviously not take as long. As with any nerve excision, there's a chance I'll have some permanent numbness (though less of a chance with this nerve) but like I said last time, I'll take numbness over pain any day.
When it's come up in conversation that I'm having another ON surgery, I've noticed the reaction most people have involves a lot of head tilting, cringing, "oh nos," and "I'm sorrys!" And I get that. Ironically, though, that sentiment couldn't be further from the emotions I'm feeling. Allow me to explain.
Imagine you just found out that you're going on an extravagent vacation. We're talking all-expenses-paid, once-in-a-lifetime, destination of choice, pinch-me-so-I-know-this-isn't-a-dream kind of trip. You're counting down the days, bursting with anticipation. You start mentioning your travel plans to friends and family and maybe even some strangers.
Here's how they react...while wincing and nodding apologetically.
"Oh gosh, I can't believe it. You poor thing...such little leg room on the plane these days. You may even have a connecting flight. I sure hope the layover isn't too long. I'm so sorry if it is!"
"Wow. Does this mean you're going to have to print your boarding pass? Are you worried about your printer running out of ink? Oh, you're going to just go electronic? Are you worried about your phone dying at the airport?"
And here's how you react:
Huh?
But now I'll throw ya a curveball. (Bear with me.)
You find out that when you board this magical plane, it's not a total guarantee that it's taking you to [insert dream destination]. I mean, there's a really good chance that it will. It's taken a lot of people who've come before you exactly where they wanted to go but, it could end up just circling your departure city, or even sitting on the tarmac for a few hours until you realize this whole thing is a bust. Ugh, imagine how deflated you'd feel returning home now? There's also a chance that it gets you from point A to point B perfectly safely, but it takes just a few hours longer than you were anticipating...and maybe there's sweaty-palm-inducing turbulence along the way. And even if everything else goes as planned, of course flying does always carry some inherent risk.
Aha, the plot thickens. Do the potential risks blunt your enthusiasm? Or does the potential reward (ahem...PARADISE) still make it no-brainer?
Do you see what I'm getting at?
Re-reading this all, I'm realizing maybe this is sort of a shitty analogy, but I'm in it too deep now. A lavish, vacation is just that; a luxury. I would never consider the mere absence of chronic pain to be a luxury. That's absurd...even if it sounds like a total dream to me. And I also don't mean to trivialize the completely legitimate apprehension someone might feel in making the decision to have their head or neck cut into. That's no joke. Oh right, and then there's equating a free trip to a surgery that you and your husband pay for out-of-pocket...again. Haha. Fun fact: insurance companies don't cover ON decompression/excision!
But I think you get the point. When you're suffering and there is a solution ahead of you...even just a probable solution...no, even just possible solution...that's all you can - and I'd argue, should - focus on. Enduring invisible pain that consumes you day in and day out without letting it just completely break you requires a tremendous amount of mental and emotional resilience, but I consider this thought process to be more about logic than grit. Just like it would be completely irrational to get bogged down by printer ink and leg room.
At the very least, you've gained some insight into my mindset but maybe - hopefully - it could help you better relate to or understand others who are suffering from chronic pain. Maybe you don't think support is all about word choice and facial expressions, but as someone who spends their days teetering back and froth over the fine line between hopeful and hopeless, I can tell you that sometimes it kind of is. Instead of someone's rocky or uncertain road to recovery eliciting sad condolences, how about an optimistic congratulations that they're on a road to recovery?
I think that's it for now. Thanks for reading as always. I'll be sure to post more after surgery in a few short weeks!